I share my life on this blog — heartfelt things and an eclectic mix of the pretty, the practical, and the pensive. This one feels more personal than most, but I’m sharing it because my subscribers asked me to.
In February 2026, my doctor removed my ovaries and fallopian tubes — a procedure called a bilateral salpingo-oophorectomy, or BSO.
What follows is simply my experience. It’s not medical advice. I may have misunderstood or may oversimplify some of the technical aspects, and every body is different. Please talk with your own doctor about your situation.
When I mentioned my upcoming surgery in an email to subscribers, I asked if anyone wanted to hear more about it. Every single person who responded said yes. A few even wrote to me privately.
When I was preparing for surgery, I read other women’s stories. They really helped me understand what to expect. So this is me paying that forward.
I have no shame in keeping things real.
Why I Chose Surgery
Years ago — completely by happenstance — an MRI for something unrelated revealed a cyst on my left ovary.
It appeared benign. Common. Nothing urgent. My doctors were thorough and confident. The typical protocol is to monitor it.
So I did for about eight years.
Every year: MRI.
Every year: “Still looks benign.”
Every year: Slight growth.
Very slow. Very steady.
By the time I decided on surgery, it measured 6 cm — larger than an egg, about the size of a small plum. That may sound dramatic, but ovarian cysts are astonishingly common. Many women have them and never know. Many cysts grow much larger than mine and never cause problems. In my case, steady growth over several years, combined with my age, made removal the wiser choice.
After menopause, ovaries no longer cycle the way they once did. Before menopause, they form functional cysts all the time, and those usually resolve on their own. A persistent cyst later in life is less likely to disappear and more likely to remain structural. When a cyst continues to grow for years in a postmenopausal ovary, doctors give it more scrutiny. And while most ovarian cysts remain benign, the overall risk of ovarian cancer increases with age. That doesn’t mean mine looked suspicious — it didn’t — but it meant watching it indefinitely no longer felt like the best long-term plan.
I sought a second opinion. Both doctors agreed: it would likely need to come out eventually, and removing it while it was still relatively small was wise. Waiting longer increases the risk of complications, including torsion (when the ovary twists and becomes an emergency).
Once I decided, I waited three months for an opening in my surgeon’s schedule.
During that wait, I became hyper-aware of my left ovary. It felt achy. Was that real or the power of suggestion? Hard to say. But it doesn’t ache anymore.
My Surgical History
I had a C-section in 1989 with my second child.
At 45, I had a hysterectomy but kept my ovaries — doctors generally recommend preserving them when possible. Ovaries continue producing hormones that support bone density, cardiovascular health, cognitive function, and overall vitality even after menopause.
The downside? Scar tissue.
Between the C-section and hysterectomy, I developed significant adhesions. Scar tissue can cause organs that should move freely to adhere to each other. In my case, my colon had adhered where it shouldn’t have been. I never had symptoms, but during this surgery my surgeon released those adhesions and removed additional scar tissue along my pelvic wall.
The Technology: Robotic Surgery
My surgeon used the da Vinci surgical robot for my surgery, a system widely used in gynecologic procedures like hysterectomies and ovary removals.
The machine itself looks like something out of science fiction. Large. Mechanical. Almost theatrical.
The surgeon does not “become” the robot. She sits several feet away at a console — almost like an advanced gaming pod — and controls the robotic arms with remarkable precision. The system allows for:
- Smaller incisions
- Greater precision
- Enhanced visualization
- Less blood loss
- Faster recovery for many patients
My surgeon made five small incisions in a slight arc across my abdomen, centered at my belly button. She placed the camera through the largest incision in my navel and removed the cyst intact through that opening. To avoid any risk of unexpected malignancy, she did not cut the cyst inside my body.
The other incisions were about an inch each.
It is laparoscopic surgery — but elevated.
What Actually Happens During Surgery
You are under general anesthesia, of course.
The surgical team places your body in what’s called the Trendelenburg position — tilted about 30 degrees with your head lower than your feet. This allows gravity to move the intestines away from the surgical field.
They inflate your abdomen with carbon dioxide gas — CO₂. Think of it as creating a balloon-like working space so the instruments can move without bumping into or damaging surrounding organs.
My surgery lasted one hour and forty minutes.
There were two doctors. My doctor removed my ovaries and fallopian tubes, released adhesions, and cleared scar tissue.
Everything was benign.
I created this AI-generated illustration for educational purposes, based on medical references.
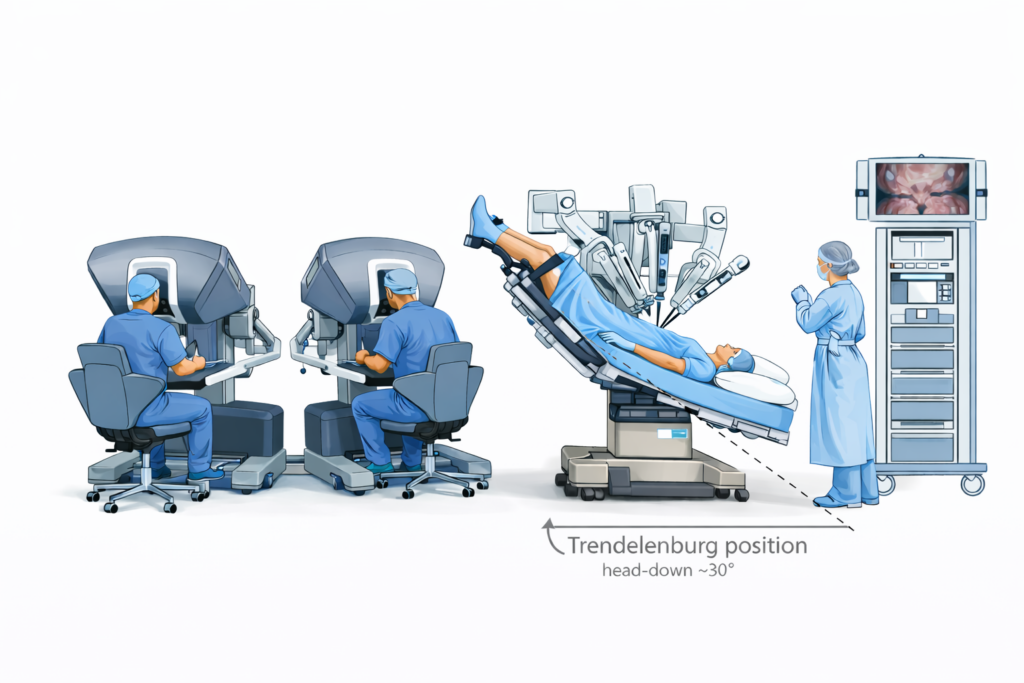
During robotic surgery with the da Vinci system, the surgical team places the body in what’s called the Trendelenburg position — head down, legs elevated — allowing gravity to gently move the intestines away from the pelvis so the surgeon can work with precision.
The Part No One Talks About Enough: The Gas
The CO₂ lingers, and your body slowly absorbs it over about two weeks or more. Until it does, it causes pain — often in the shoulders and back as CO₂ rises. I also had pain in my neck and upper abdomen, well above the incisions.
Walking helps.
Movement helps.
Time helps.
When I got home, between the swelling from surgery and the remaining gas, I felt like I looked about five months pregnant. They remove as much gas as possible, but they can’t remove it all.
The gas is not in your intestines, so GasX or other typical gas remedies do not work. Your body simply needs time to absorb it.
For pain, my care team instructed me to take 1,000 milligrams of acetaminophen together with 600 milligrams of ibuprofen every six hours for three days — literally together. The bottle even read, “Take one tablet by mouth every six hours with acetaminophen for 3 days.” It felt like a lot at first, but it worked, and it reminded me that even outpatient surgery is still surgery. I also took three doses of oxycodone when the pain spiked higher than the rotation could handle.
I arrived at the hospital at 10:45 a.m. for intake and was home by 6:00 p.m.
Recovery (The Honest Version)
You’ll hear “two weeks.”
That’s partially true.
Two weeks to feel fairly normal. At the time of this writing, I’m nearly three weeks post-surgery. I’m still a bit sore and had to be careful lifting groceries today. But I’m really back to normal otherwise.
Full internal healing per my doctor is 4–6 months.
Some women return to work within days. Others need several weeks. So 1–4 weeks is the average time it takes to feel back to par.
I’m retired with no obligations, so I rested easily.
I lounged. I binged Netflix. I sipped tea. I walked around the house because movement helps the gas dissipate.
Mostly, I felt exhausted. And those first several days were a blur.
On Day 9, Valentine’s Day, Ron and I attended a special showing of Swan Lake in San Francisco. The ballet!
Perhaps not a smart move so close to surgery, but we had purchased orchestra seat tickets long before surgery was on the calendar. We had reservations at the luxurious Palace Hotel and dinner reservations at Le Central, an upscale French restaurant.
I really wanted that evening.
The whole night proved elegant and romantic. I’m so glad we went.
And then for two days afterward, I slept — a lot.
Totally worth it.
A Side Conversation That Matters: Vaginal Estrogen
Before surgery, I experienced cramp-like sensations that felt unusual for someone past menopause. I also had other symptoms. This wasn’t the reason for my surgery, but it did lead to further conversations with my doctor.
I learned that I needed localized vaginal estrogen cream, available by prescription. Many physicians recommend it for women over 50 and advise continuing it long term — even indefinitely. That’s not a typo.
No one talks about this enough. I’ll share more about that in a separate post This Is Not Your Mother’s Hormone Therapy — Aging Changes Can Be Treated Safely.
The cream made a significant difference for me. I feel better — on several levels.
If you have questions about my experience, I’m an open book. You can always send me a personal note.
I share these resources for informational purposes only. Please consult your physician before beginning any medical treatment.
Excellent Care at Kaiser Permanente Medical Center
I cannot say enough about the wonderful care I received during my surgery — and always.
I felt and feel profoundly cared for.
It takes an astonishing number of professionals to move one human safely through surgery — from symptom to recovery. I appreciate every detail—from preop to recovery. I never felt like a number. Everyone treated me with such kindness and gentleness. And the air-warmed blanket is cloud-like. Honestly, it surpasses a spa experience. Its weightlessness and efficiency always amaze me.
I wrote handwritten thank-you cards to several people afterward because my verbal thank-yous felt insufficient. If I experience something positive, you can bet you’ll hear from me.
I feel incredibly fortunate for wonderful professionals and healthcare.
If you’re walking through something similar, I hope my information gave you clarity. In my experience, it was very manageable.
Be well. My best to you. 🦋
If you’d like to receive the posts and surveys I send to subscribers, you can join here.


4 comments
Thank you for sharing. I’m so sorry you had to go through this. I am happy that it turned ok for you. Stay blessed, my friend.
Thank you. It’s a very common surgery and I hope women find my experience useful. 🌷
Thank you for sharing! I’m glad that we are all starting to be more open and talk about things like this. It definitely helps!
I’m glad surgery went well, and I hope you continue to heal and rest!
Thank you, Emily, for your well wishes 💐. Several people have reached out to me to connect, share, and ask questions. I’m so happy I have this platform for exactly that. Stay tuned next week for an even more personal, feminine issue; one that all women need to know about. I hope you’re making it a great day. 🌈